Dry skin in babies and children
It’s common for babies and children to have dry skin. However, dry skin can also be easy to prevent and treat with a little care and attention. Dry skin can be a condition on its own, or also be a symptom of something else which maybe going on in the baby’s body. Either way, it can be helpful to understand some of the more common causes of dry skin and what can help in its management.
Table of Contents
Most common reasons for dry skin
Babies who are born overdue are prone to dry, flaking skin. This can be obvious from birth, but it can also become more apparent in the newborn period. Dry skin in babies who were ‘post-dates’ or overdue is caused when the protective layer of vernix caseosa starts to deplete as a baby approaches their due date. Vernix helps to protect the baby’s skin, much like a waterproof coating, causing it to be softer and smoother at birth and after the baby is born. Being post due or overdue means the baby’s skin is more exposed to the amniotic fluid.
Other causes for dry skin:
- Irritation from drying bathing agents. Soap, strongly perfumed baby wash, bubble bath and occasionally, ‘botanically’ sourced products can be irritating to a baby’s fragile and sensitive skin.
- Exposure to moisture – this is common in babies who are drooling a lot e.g., when they are teething. Sometimes a ‘dribble’ rash extends down the chin and into the skin folds on the neck. This is because there less opportunity for the skin to stay dry where there’s limited air flow.
- Bathing too frequently can cause the skin to lose its natural, protective oils. Once they’re washed off, the skin can’t hold moisture and dries out.
- Climate – in dry climates, there is a greater tendency for dry skin. There is also more likelihood of the skin drying out during cold, dry weather when both the temperature and the humidity are low.
- Family history – where other family members are prone to dry skin, it’s not unusual for their babies to be affected by the same genetic influence.
- Skin conditions – Eczema, Keratosis Pilaris, Pityriasis Alba amongst other skin conditions, can cause dry/rough/pale spots on the skin.
How to prevent dry skin
It can be hard to prevent dry skin, but these strategies are often useful:
Bath your baby daily or a few times each week. Avoid giving them long, soaking baths – around 5-10 minutes is generally enough time to be in water. Use warm water in their bath and first, test the temperature on your wrist or forearm.
Choose bath products which are unfragranced and match the pH of a baby’s skin – the ideal pH level of a baby’s skin is 5.5. Choose a baby bath wash which is mild and intended for babies and/or children.
After your baby’s bath, pat their skin dry using a soft and absorbent towel. Keep your baby’s towel separate from the rest of the family’s. Pay particular attention to your baby’s skin folds and pat dry.
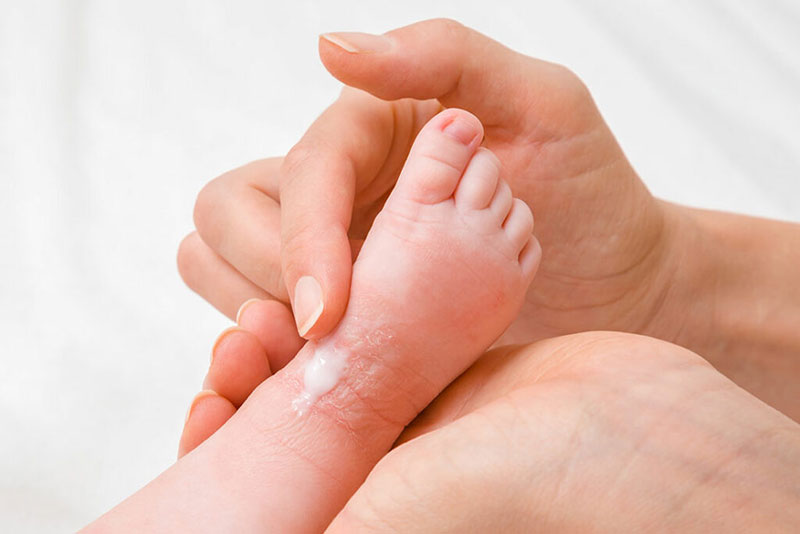
Apply a non-fragranced lotion or moisturiser to your baby’s skin shortly after drying them. While their pores are still open and the skin warm and slightly moist is the best time for moisturisers to be absorbed.
How to manage eczema
Experts estimate that around 1 in 4 Australian children are affected by eczema, a skin condition which usually starts at less than 12 months of age. Eczema tends to follow patterns of flaring up and then improving until, by school age, most children have grown out of it.
- If you suspect your baby has eczema, have them checked by your doctor. There are a number of reasons for dry skin and it’s important to have a correct diagnosis first.
- Keep your baby’s fingernails short so they can’t scratch and cause further skin irritation.
- Dress your baby in cotton or natural fibres. Avoid dressing them in rough, scratchy or tight clothes.
- Use hypoallergenic products where possible.
- Apply a moisturiser within three minutes of bathing to help ‘lock in’ the moisture in their skin.
- Gently pat, not rub their skin dry after bathing.
- Use sensitive skin washing powders and detergents.
- Avoid rapid changes in temperature and your baby overheating.
- Rinse or bath your child after swimming. Chlorine and/or salt can be especially irritating.
- Avoid their skin being exposed to irritants like grass, sand or carpets/rugs.
Don’t forget to moisturise!
Ideally, eczema is kept under control by keeping the skin moisturised, which helps to improve the skin barrier.
- In-between bathing, at least 1-2 times a day, it can help to moisturise the baby’s whole body.
- As a general guide, the thicker the cream the better it is on dry skin. Creams also tend to be more moisturising than lotions and are less likely to sting.
Treating eczema
Be guided by your doctor when making decisions about treating your baby’s eczema. Every baby is an individual and what is right for one may not be right for another.
As a general guide:
Anything that reduces humidity can lead to dry skin – this includes air conditioning, central heating or wood burners. Dry skin worsens in the winter months because there is less humidity and more chance that the central heating is on.
- Use steroid of other (prescribed) creams as prescribed and recommended.
- Be mindful of hygiene when using creams and lotions and avoid ‘double dipping’ your fingers into tubs and tubes. Instead, use a spatula or cotton tip to dispense what you need.
- Wash your hands after applying prescribed creams to your baby’s skin.
- Be mindful that steroid ointments are often preferred as they are more moisturising and often more effective.
- Apply topical creams liberally, so all of the eczema is covered.
- Keep the child’s skin cool and avoid them becoming overheated.
- In cases of severe eczema, wet dressings may be recommended, especially if a child is scratching and waking at night.
For more information on eczema, check Eczema Association Australia (eaa).
Written for E45 by Jane Barry, Midwife and Child Health Nurse, March 2023.
























