Psoriasis
Psoriasis is an inflammatory skin condition that affects roughly 2% of the UK population.
What is it and how do I manage it?
Psoriasis is an inflammatory skin condition that affects roughly 2% of the UK population. There are different types of psoriasis and the symptoms can range from mild to severe, so it can vary a lot from person to person.
Although there is no cure for psoriasis, you might find you go through periods when it is better and times when it flares-up. Psoriasis can also affect more than the skin – you might find it has an impact on your nails or joints too. Knowing what type of psoriasis you have is important when it comes to finding the right treatment.
Psoriasis can happen at any age, but most often starts between the ages of 10 and 35. It may also be associated with other medical conditions such as diabetes, heart disease, Crohn’s disease, obesity, anxiety and depression.
Types of psoriasis
There are a number of different types of psoriasis, but the following are the most common.
Plaque Psoriasis
Plaque psoriasis is by far the most common type of psoriasis, affecting 9 out of 10 sufferers. It is also known as psoriasis vulgaris. Normal skin cells are replaced every 3-4 weeks but in psoriasis this happens every 3-4 days. This is thought to be due to genetics and environmental factors.
Plaque psoriasis appears as well-defined patches of irregularly shaped, or oval, pink-red skin covered in silver-white scales (referred to as ‘plaques’). The thickness of the scales can vary. On darker skin the plaques may be grey coloured. The plaques are most often on the forearms, shins, knees, elbows, scalp, behind the ears, on the torso and around the buttocks. The skin may be itchy, but not usually sore, and can also crack – especially if the palm of the hands or soles of the feet are affected.
While it is a long-term condition, around 1 in 4 people with plaque psoriasis can find it goes away for months at a time.
Erythrodermic psoriasis
Erythrodermic psoriasis is a rare, potentially life-threatening type of psoriasis. It is thought be caused by genetics and some environmental factors. Erythrodermic psoriasis can develop gradually or come on suddenly – spreading across the whole body to affect more than 90% of the skin. You might also feel unwell with fatigue, fever and develop swollen lower legs. If you have these symptoms you should go straight to A&E.
Erythrodermic psoriasis can happen in anyone with plaque psoriasis but can be triggered by factors like infections or skin irritants.
Flexural psoriasis
Flexural psoriasis, also known as inverse psoriasis, affects the creases and folds of your skin. It can cause itchy, red, glazed areas in your skin folds, such as the armpits, groin, genitals, buttocks and under the breasts. Sweat or rubbing the affected skin can cause further irritation. The condition is more common in people who are overweight, immobile or elderly. You may also find you’re more prone to developing yeast infections in the same areas as your flexural psoriasis.
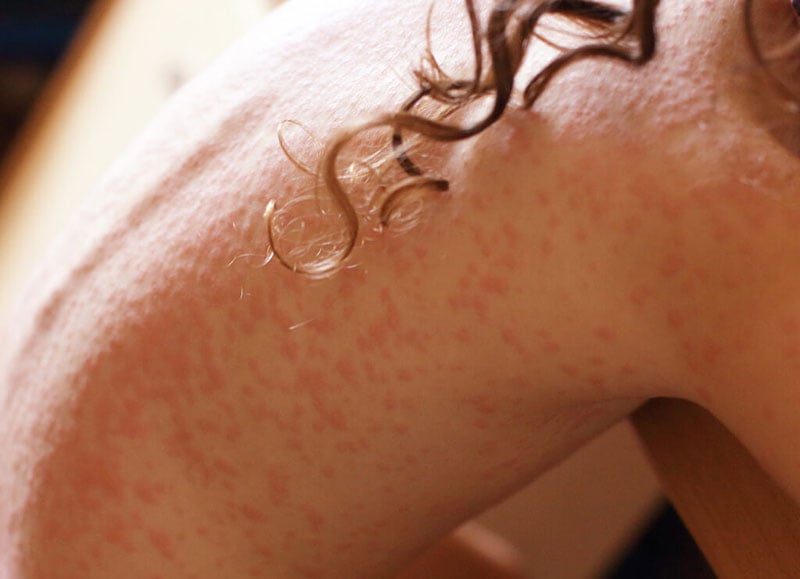
Guttate Psoriasis
This form of psoriasis is also known as ‘raindrop’ or ‘droplet’ psoriasis because it looks like droplets on the skin. Certain people who have had guttate psoriasis will develop chronic plaque psoriasis later in their life. Guttate Psoriasis most frequently occurs in children and teenagers, usually after a throat infection caused by streptococcal bacteria. Even though it may be caused by an infection, guttate psoriasis is not contagious. The condition develops over the course of a week, with many small, raised, scaly patches that are round or oval and pink or red appearing all over the body.
Nail psoriasis
Nail psoriasis affects the fingernails and toenails with a range of symptoms. Nails may turn orange-yellow, become pitted, start to come away from your skin or disintegrate. The condition is more likely to affect your fingernails than your toenails. Nail psoriasis can happen in anyone with psoriasis, but it is particularly common if you also have arthritis-associated psoriasis.
Pustular Psoriasis
This is a rare type of psoriasis where there are pus-filled spots on or surrounded by red skin. There are two main types of pustular psoriasis: generalised and localised. Around 5% of people with psoriasis experience localised pustular psoriasis, but in rare cases this can be generalised which can be life threatening. Localised pustular psoriasis (also known as palmoplantar psoriasis) appears as yellow-brown blisters, known as ‘pustules’, on your palms and soles along with scaly skin and redness on your toes and fingertips. In generalised pustular psoriasis, redness spreads quickly over your skin followed by the development of multiple white pustules that group together to form large areas of pus. These blisters are not contagious.
Pustular psoriasis is more common in those who have, or have had, plaque psoriasis. However, you can develop it even if you’ve never had psoriasis before. Triggers range from stress, certain medicines and infections to pregnancy or too much sun. Localised pustular psoriasis usually occurs in those aged 20-60, particularly if you smoke.
Scalp Psoriasis
Scalp psoriasis looks like plaque psoriasis, but affects your scalp. Your hair traps the scale making it hard to rub away, and as a result the plaques can become thick. Some people find that only parts of their scalp is affected, while for others it’s across their whole scalp. In some cases scalp psoriasis can even cause bald patches, but the hair will normally grow back. Up to 9 out of 10 people with psoriasis develop it on their scalp. Some people may experience itchy scalp, a feeling of tight skin and occasionally soreness if the skin cracks.

General symptoms of psoriasis
Although there are many different types of psoriasis with different symptoms, most people have plaque psoriasis. Around 80% of those with psoriasis have a mild form where just a few areas of skin are affected and can be easily managed. You may experience some, or all, of the following psoriasis symptoms, depending on severity and type:
- Dryness
- Cracked skin
- Blisters/ pustules
- Red skin
- Bleeding skin
- Itchy skin
- Sore painful skin
- Skin build-up / Silver scaly skin
- Glazed skin
Psoriasis triggers and factors
Although psoriasis can be a genetic condition, there are many other reasons why you can develop it – or triggers that can make it flare up. Here are the common triggers that can either bring on psoriasis, or cause a flare-up if you already have it.
Medications
Medicines that can cause or trigger psoriasis include:
- Lithium
- Anti-malarial drugs
- Some blood pressure drugs, such as beta-blockers and ACE inhibitors
- Coming off steroids too quickly, like prednisone
- Some antibiotics, like penicillin and tetracycline
- Non-steroidal anti-inflammatory drugs
- Some anti-depressants, like trazodone
Stopping steroid medicines suddenly can trigger pustular or erythrodermic psoriasis.
How to avoid:
Speak to your doctor or pharmacist about starting or stopping these medicines in case they affect your psoriasis.
Injury
Damage to the skin from scratches, burns, insect bites, piercings, tattoos or sunburn can trigger psoriasis. Also known as the ‘Koebner phenomenon’, this happens in about 20% of people with psoriasis – with symptoms developing about 1-2 weeks after the skin is damaged.
How to avoid
- Treat any skin injuries quickly
- To avoid being bitten, cover up and use insect repellent or stay indoors at dawn and dusk when insects are most active
- Think about whether a piercing or tattoo is worth the risk
- Try to avoid scratching itchy skin as this alone can trigger a flare-up
- Wear sunscreen, ideally one that is a broad-spectrum sunscreen with SPF 30 or higher, and water resistant
- Try to avoid cuts when shaving by putting a moisturizer under your shaving cream.
Lifestyle
Smoking and excessive or frequent drinking can make your psoriasis flare up. Localised pustular psoriasis usually only develops in smokers. Those who drink too much may find this makes their psoriasis treatment less effective. Being overweight increases your chances of developing flexural psoriasis.
How to avoid:
- Stop smoking and moderate your drinking. Pharmacists can offer advice on how to cut down and stop smoking
- Limit the time you spend around smokers
- Weight loss can help if you have flexural psoriasis but also helps reduce your risk of heart disease. You can ask your healthcare practitioner for guidance and support.
Stress
Stress is a common psoriasis trigger.
How to avoid
- Try relaxation techniques, such as deep breathing, yoga, tai chi or meditation
- Use distraction methods such as baking, knitting, or painting – whatever works for you
- Get a good night’s sleep. To help, try having a relaxing bath or shower before bed, avoid electronic devices for an hour or two before bedtime and sleep in a dark, cool room
- Exercise regularly
- If you feel you can’t manage your stress, talk to a healthcare professional.
Weather
Weather can be a trigger – both dry, cold weather or too much sun can cause a flare in some people with psoriasis. However, for some people, sunlight can help improve their psoriasis.
How to avoid
- Use humidifiers to put moisture back into the air and avoid air conditioning
- Don’t sit close to radiators or fires
- Protect your skin from extreme cold by wearing winter clothing, including hats and gloves
- Wear sunscreen to reduce the risk of sunburn
- Apply a moisturizer throughout the day when your skin feels dry
- Limit showers and baths to 10 minutes; use warm water rather than hot water.
How to manage psoriasis
As well as avoiding triggers that can cause flare-up, there are many ways you can manage your psoriasis.
Emollients
Emollients are moisturisers that can help reduce the scaling and itching caused by psoriasis. Not only can make your skin look better by removing scales, it can also make it easier to apply other psoriasis treatments – and may even help them get deeper into your skin. Emollients also soften your psoriasis skin, soothing it and can make it less likely to crack.
Applying emollients regularly can help keep you manage your psoriasis by:
- Replacing the lost water in your skin
- Helping to restore a healthy skin barrier
- This, in turn, helps protect the skin from damaging irritants and allergens.
Some emollients may contain extra ingredients to help control itchiness.
As regular soaps and cleansers can irritate the skin and cause dryness, it’s important to wash with an emollient too. There are special emollients that can be used for washing just as you would use soap, or you can apply your leave-on emollient as a soap substitute. Be prepared though – while emollient soap substitutes clean effectively, they don’t lather up like regular soap. You can also add emollients to your bath.
Coal tar
Coal tar can help reduce scale and inflammation when you have psoriasis. It can be applied to the skin, or coal tar-containing bath products and shampoos (for treating scalp psoriasis) are available over-the-counter to buy.
Steroids
Topical corticosteroids help reduce inflammation in psoriasis. You shouldn’t use over-the-counter steroid creams and ointments to treat psoriasis unless told to by your doctor or treating specialist. They will know the right strength of steroid needed for your case.
If you are using steroids, you should continue applying your emollients. Apply your emollient first, followed by your steroid cream or ointment 20-30 minutes after.
Prescription medicines
There are other treatments that your doctor or specialist dermatologist can prescribe. These are usually products you can apply to your skin, such as strong steroids, coal tar, vitamin D based treatment, biologic agents or dithranol.
A person’s treatment plan should be created by their doctor based on their specific needs.
























